The ring that an evaporating drop of coffee leaves on the counter might be the solution to saving hundreds of thousands of lives.

Research accelerating at Vanderbilt offers new hope in diagnostics for malaria and other diseases. The interdisciplinary team is led by Professor of Biomedical Engineering Rick Haselton, Stevenson Professor of Chemistry David Wright, and Biochemistry Associate Professor Ray Mernaugh, and includes two other biomedical engineering faculty, three postdoctoral and six graduate students.
“We intend to produce a diagnostic platform to measure common clinical chemistry biomarkers,” Haselton said. “It is our hope that this platform will ultimately reduce the burden of diseases like malaria and tuberculosis by improving early diagnosis and ensuring proper treatment.”
The goal is to create point-of-care diagnostics that can be used in developing areas.
The team is designing a simple blood test to determine if someone is infected with the malaria-causing Plasmodium parasites. Swift and accurate malaria diagnosis would allow for faster treatment and save more lives. Malaria kills more than half a million people every year, the vast majority young children in sub-Saharan Africa.
The microscopic characteristics of malaria in a blood sample are telltale, which should enable relative fast and accurate diagnosis. Unfortunately, conventional tests require refrigeration, electricity and an experienced medical technician – all often in short supply in developing countries where malaria rages most furiously.
The idea for the Vanderbilt team’s “coffee ring” biomarker detection process came when they sought naturally occurring phenomena that could be engaged to detect malaria.
The researchers considered how coffee evaporating on a flat surface leaves behind particles visible with the naked eye and wondered if malaria indicators in a blood sample could be induced to do the same.
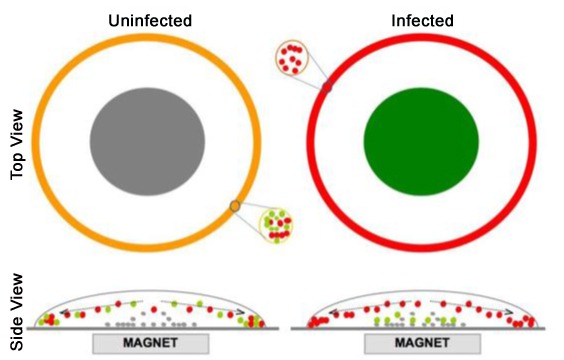
Their proposed malaria test consists of a specially developed liquid and glass slide containing a small magnet. The liquid is mixed with the blood sample and a drop of that mixture is placed on the glass slide. Once it has dried, the color pattern of the resulting ring indicates a positive or negative test. If the ring is yellow, the person is not infected. If the ring is read with a green center, the person has malaria.
The test does not require refrigeration or a lot of training to administer, making it viable even in the poorest areas, said team member and postdoctoral fellow Josh Trantum, BE’95, MS’10, PhD’13, whose Ph.D. focused exclusively on the research.
When local health workers lack resources, a malaria diagnosis may be based on symptomatic factors including fever, leaving asymptomatic patients undiagnosed. People can transmit the Plasmodium parasite without possessing significant symptoms.

Trantum reported that the team is currently doing well against project goals. “We published a version of the coffee-ring diagnostic in the Royal Society of Chemistry’s Lab on a Chip (Nov. 2013) that is capable of producing a clinically-relevant limit-of-detection. Our team is now busy working on a field-deployable form factor as well as adapting the diagnostic design to various disease targets,” he said.
“The new field-deployable technology could ultimately quickly identify more cases, leading to more treatment, reducing transmission, and dramatically increasing eradication efforts,” Trantum said. “This could be very good global-health news.”
The project has been supported by the Vanderbilt Discovery Grant Program and a Grand Challenges Exploration grant from the Bill & Melinda Gates Foundation.
Contact:
Brenda Ellis, (615) 343-6314
Brenda.Ellis@Vanderbilt.edu
Twitter @VUEngineering